Did the COVID-19 lockdowns reduce air pollution in Lombardy?
Air pollution is currently the most important environmental risk to human healt in Europe [1]. Exposure to fine particulate matter (PM2.5) and nitrogen dioxide (NO2) increases mortality rates and hospitalizations due to respiratory and cardiovascular disease [2]–[7], and it leads to a decline in physical and cognitive productivity [8]–[12].
Lombardy is one of the most polluted regions in OECD countries. Did its inhabitants breath cleaner air during the COVID-19 lockdown from March 6 to May 4, 2020?
Using a machine-learning algorithm, researchers at the the European Institute on Economics (EIEE) and the Environment, Bocconi University and Politecnico di Milano estimated that the lockdown from March to May reduced background concentrations of PM2.5 by 3.84 µg/m3 (16%) and NO2 by 10.85 µg/m3 (33%). Nonetheless, the improvement in air quality saved at least 11% of the years of life lost and 19% of the premature deaths attributable to COVID-19 in the region during the same period.
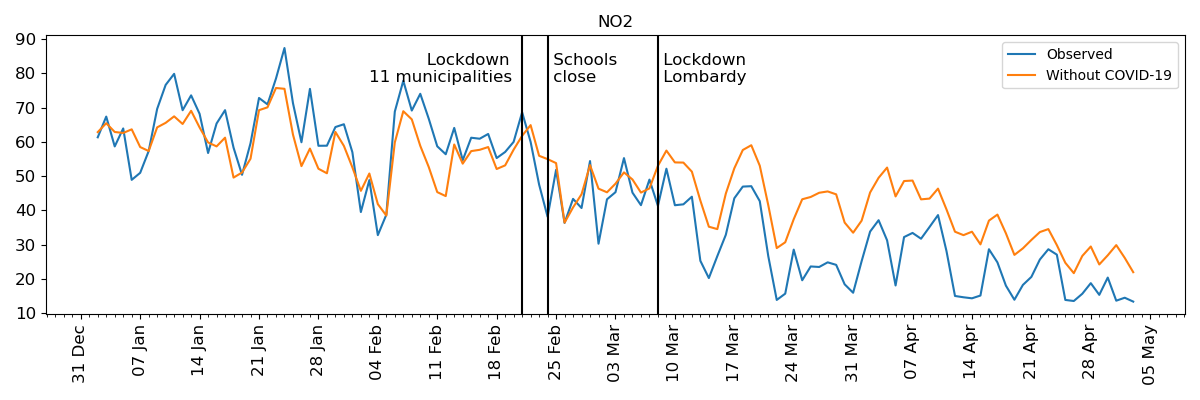
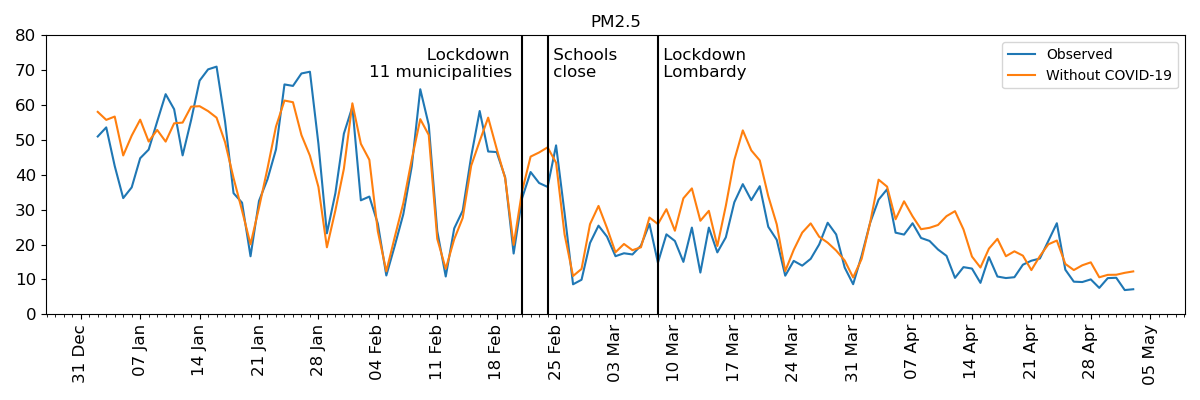
| PM 2.5 | NO2 | |
|---|---|---|
| Avoided premature deaths/100.000 inhab | 10.2 to 24.8 | 28.8 |
| as % of COVID-19 premature deaths | 6.5% to 16% | 18.60% |
| Years of life saved/100.000 inhab | 72.1 to 175.9 | 203.7 |
| as % of COVID-19 years of life lost | 3.8% to 9.3% | 10.8% |
Avoided premature deaths and years of life saved for PM 2.5 are calculated using hazard ratios from Krewski et al. (2009) (lower bound) and Lepeule et al. (2012) (upper bound). Calculations for NO2 use an hazard ratio from Henschel et al. (2018). Avoided premature deaths are calculated using the population-weighted change in concentrations at background stations. Given the high correlation between concentrations of PM2.5 and NO2, the concentration-response function of these pollutants are interdependent. It is recommended that avoided deaths and YLS be not aggregated across pollutants, lest incurring in partial double counting. For comparison, in Lombardy, from February 22 to May 3 2020, every 100,000 people 155 died after testing positive for COVID-19 and 1891 years of life have been directly lost to the virus.
Concentrations of PM2.5 and NO2 since November
The same methodology is applied to track the effect of the second COVID-19 lockdown on concentrations of PM2.5 and NO2.
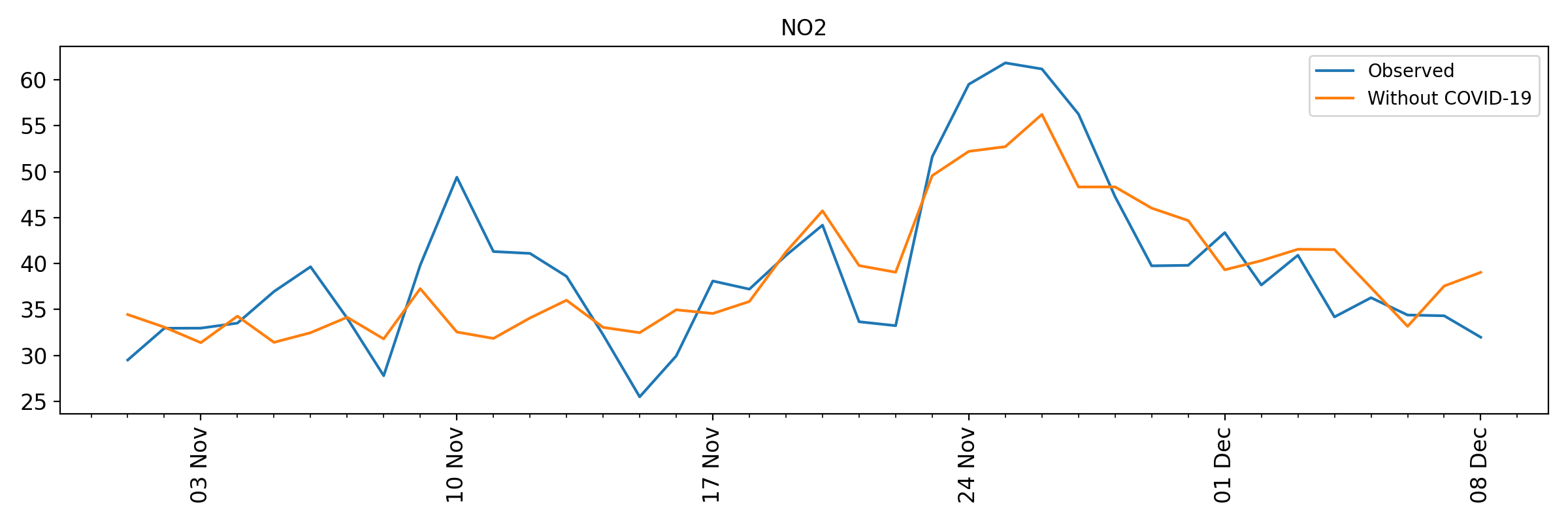
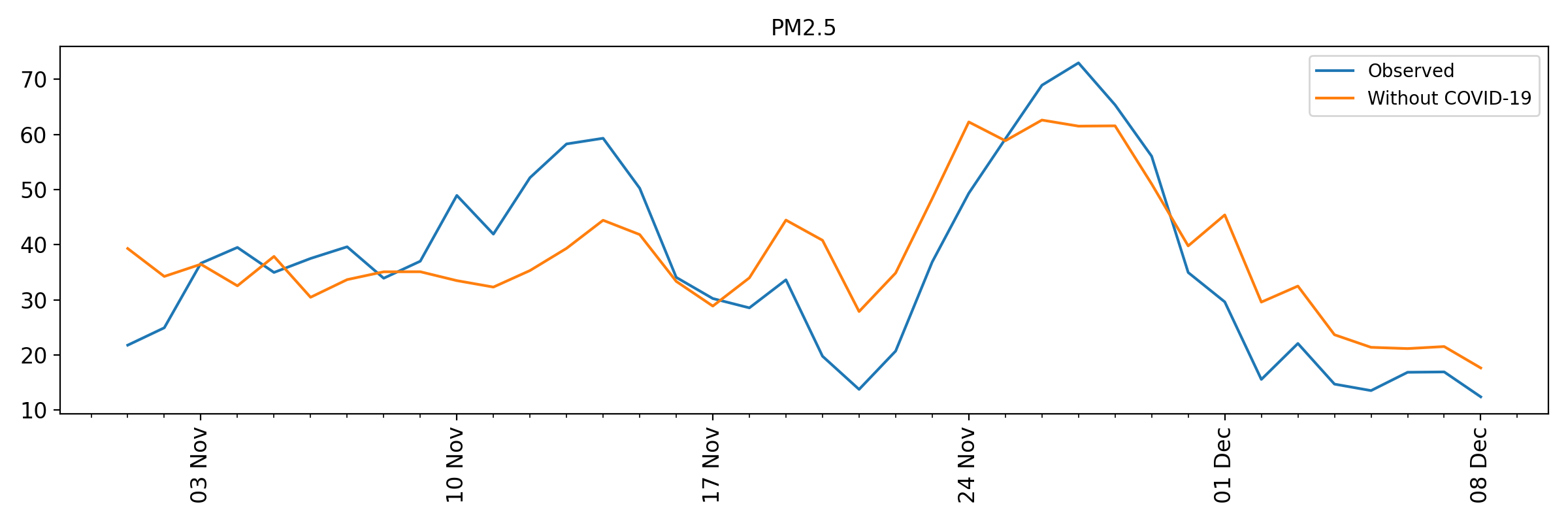
Methodology
The methodology is described in “COVID-19 lockdown only partially alleviates health impacts of air pollution in Northern Italy”, by Francesco Granella, Lara Aleluia Reis, Valentina Bosetti and Massimo Tavoni, published on Environmental Research Letters.
Contacts
Francesco Granella - Bocconi University and RFF-CMCC European Institute on Economics and the Environment
Lara Aleluia Reis - RFF-CMCC European Institute on Economics and the Environment
Valentina Bosetti - Bocconi University and RFF-CMCC European Institute on Economics and the Environment
Massimo Tavoni - Politecnico di Milano and RFF-CMCC European Institute on Economics and the Environment

References
[1] European Environment Agency, Air quality in europe - 2019 report. European Environment Agency, 2019.
[2] C. A. I. Pope and D. W. Dockery, “Health Effects of Fine Particulate Air Pollution: Lines that Connect,” Journal of the Air & Waste Management Association, vol. 56, no. 6, pp. 709–742, Jun. 2006.
[3] A. Ebenstein, M. Fan, M. Greenstone, G. He, and M. Zhou, “New evidence on the impact of sustained exposure to air pollution on life expectancy from China’s Huai River Policy,” Proceedings of the National Academy of Sciences, vol. 114, no. 39, pp. 10384–10389, Sep. 2017.
[4] T. Deryugina, G. Heutel, N. H. Miller, D. Molitor, and J. Reif, “The Mortality and Medical Costs of Air Pollution: Evidence from Changes in Wind Direction,” American Economic Review, vol. 109, no. 12, pp. 4178–4219, Dec. 2019.
[5] I. C. Mills, R. W. Atkinson, S. Kang, H. Walton, and H. Anderson, “Quantitative systematic review of the associations between short-term exposure to nitrogen dioxide and mortality and hospital admissions,” BMJ open, vol. 5, no. 5, 2015.
[6] H. Amini, N. T. T. Nhung, C. Schindler, M. Yunesian, V. Hosseini, M. Shamsipour, M. S. Hassanvand, Y. Mohammadi, F. Farzadfar, A. M. Vicedo-Cabrera, and others, “Short-term associations between daily mortality and ambient particulate matter, nitrogen dioxide, and the air quality index in a Middle Eastern megacity,” Environmental Pollution, vol. 254, p. 113121, 2019.
[7] Y. Duan, Y. Liao, H. Li, S. Yan, Z. Zhao, S. Yu, Y. Fu, Z. Wang, P. Yin, J. Cheng, and others, “Effect of changes in season and temperature on cardiovascular mortality associated with nitrogen dioxide air pollution in Shenzhen, China,” Science of The Total Environment, vol. 697, p. 134051, 2019.
[8] J. Graff Zivin and M. Neidell, “The Impact of Pollution on Worker Productivity,” American Economic Review, vol. 102, no. 7, pp. 3652–3673, Dec. 2012.
[9] A. Ebenstein, V. Lavy, and S. Roth, “The long-run economic consequences of high-stakes examinations: Evidence from transitory variation in pollution,” American Economic Journal: Applied Economics, vol. 8, no. 4, pp. 36–65, 2016.
[10] X. Zhang, X. Chen, and X. Zhang, “The impact of exposure to air pollution on cognitive performance,” Proceedings of the National Academy of Sciences, vol. 115, no. 37, pp. 9193–9197, Sep. 2018.
[11] J. He, H. Liu, and A. Salvo, “Severe Air Pollution and Labor Productivity: Evidence from Industrial Towns in China,” American Economic Journal: Applied Economics, vol. 11, no. 1, pp. 173–201, Jan. 2019.
[12] M. E. Kahn and P. Li, “Air pollution lowers high skill public sector worker productivity in China,” Environmental Research Letters, vol. 15, no. 8, p. 084003, Jul. 2020.
[13] D. Krewski, M. Jerrett, R. T. Burnett, R. Ma, E. Hughes, Y. Shi, M. C. Turner, C. A. Pope III, G. Thurston, E. E. Calle, and others, Extended follow-up and spatial analysis of the american cancer society study linking particulate air pollution and mortality. Health Effects Institute Boston, MA, 2009.
[14] J. Lepeule, F. Laden, D. Dockery, and J. Schwartz, “Chronic exposure to fine particles and mortality: an extended follow-up of the Harvard Six Cities study from 1974 to 2009,” Environmental health perspectives, vol. 120, no. 7, pp. 965–970, 2012.
[15] S. Henschel, G. Chan, W. H. Organization, and others, “Health risks of air pollution in europe-hrapie project: New emerging risks to health from air pollution-results from the survey of experts,” 2013.